Auto-Immune Blood Disorders in Dogs and Cats: Causes, Symptoms, and How We Treat Them
Sometimes the most dangerous threat to your pet’s health comes from inside their own body. Auto-immune blood diseases occur when the immune system mistakenly identifies healthy blood cells as foreign and begins destroying them. The two most common forms are immune-mediated hemolytic anemia (IMHA), where red blood cells are targeted, and immune-mediated thrombocytopenia (ITP), where the body destroys its own platelets. Both conditions can escalate rapidly, making early recognition and prompt treatment essential.
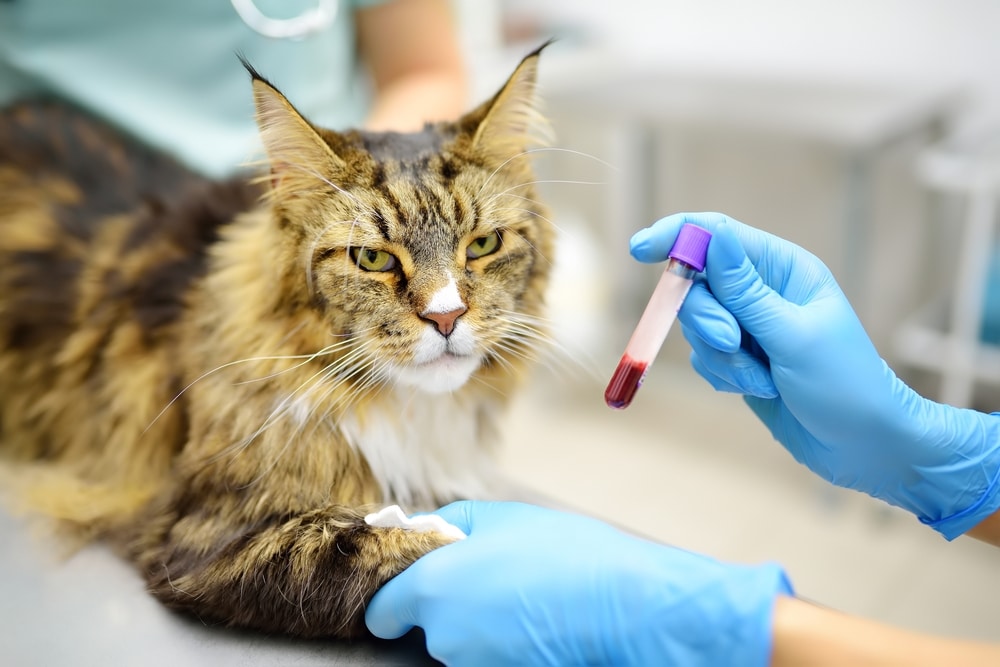
At Mid-Valley Veterinary Hospital, our diagnostic services include in-house blood work and cytology reviewed by board-certified pathologists, which means we can identify these conditions quickly and start treatment without delay. In the Central Valley, tick-borne diseases that can trigger auto-immune blood disorders are a real concern, and we screen for those as part of our workup. If your pet is showing signs of fatigue, pale gums, or unexplained bleeding, contact us right away to schedule an evaluation.
When the Immune System Turns on the Blood
The immune system’s job is to identify and eliminate genuine threats. Anemia develops when this system goes wrong and the body destroys its own red blood cells faster than it can replace them. Without adequate red cells to carry oxygen, tissues become starved, pets become exhausted, and the heart works harder trying to compensate for what is not there.
The mechanism varies. In some cases, immune complexes deposit in blood vessel walls and trigger inflammation and destruction. In others, cytotoxic antibodies attach directly to blood cell surfaces and mark them for destruction. In either case, the result is a body actively working against itself, often with alarming speed.
Immune-Mediated Hemolytic Anemia (IMHA): What It Looks Like
Recognizing IMHA Symptoms Before They Become a Crisis
Immune-mediated hemolytic anemia occurs when antibodies attach to red blood cells and flag them for destruction. As the red cell count falls, oxygen delivery throughout the body fails, and symptoms progress from subtle to unmistakable.
Early and progressive signs of IMHA:
- Unusual tiredness, reduced interest in activity or play
- Faster-than-normal breathing even at rest
- Pale or jaundiced gums (yellow tinge indicates that broken-down red blood cells are releasing bilirubin into the body)
- Dark, brownish, or reddish urine from hemoglobin being filtered through the kidneys
- Reduced or absent appetite
- Rapid or irregular heartbeat
Some breeds carry a higher breed predisposition to IMHA. Cocker Spaniels, Irish Setters, and certain other breeds develop this condition at higher rates, making owner awareness particularly valuable for those households.
Blood Clotting Complications: The Hidden Danger
IMHA carries a paradox that catches many owners off guard. While red blood cells are being destroyed, the clotting system simultaneously becomes dysregulated, creating a real risk of dangerous clot formation in the lungs, abdomen, or limbs. Blood clotting complications are one of the most serious secondary risks associated with IMHA and a leading cause of death in affected dogs.
Signs of possible clot formation requiring immediate attention:
- Sudden difficulty breathing or respiratory distress
- Limb pain, swelling, or a limb that is cold compared to others
- Collapse or sudden severe weakness
These signs require emergency evaluation without delay. During our open hours, call us at (530) 865-5634 and let us know what you are observing so we can prepare for your arrival. After hours, please contact the nearest 24-hour emergency facility.
Immune-Mediated Thrombocytopenia (IMT): When Platelets Are the Target
Immune-mediated thrombocytopenia (IMTP) occurs when the immune system destroys platelets, the cell fragments responsible for initiating clot formation at injury sites. Without adequate platelets, the blood cannot clot properly, and bleeding becomes a serious risk.
Signs of IMTP:
- Unexplained bruising on the belly, inner thighs, or gums
- Tiny pinpoint red or purple spots on the skin or gums (petechiae), often visible on the belly or inside the mouth
- Nosebleeds without a clear cause
- Blood in the urine or stool
- Cuts or minor wounds that bleed disproportionately long
IMTP is particularly dangerous because bleeding can occur internally without any visible external sign. A dog that appears to have a mild bruise may actually be bleeding into body cavities.
Evans Syndrome: When Both Systems Are Attacked at Once
Some pets face simultaneous immune attacks on both red blood cells and platelets, a combination known as Evans syndrome. This presents as concurrent immune-mediated conditions requiring treatment that manages both components together, since treating one without accounting for the other can worsen the overall picture.
Evans syndrome cases tend to be more challenging to stabilize and require careful monitoring as treatment is adjusted based on how each component responds. This is one of the situations where rapid, comprehensive diagnostics matter most, since knowing the full picture from the start shapes the entire treatment approach. Our team handles these complex cases with the individual attention and regular monitoring they require.
Tick-Borne Diseases and Secondary Blood Disorders
In rural Northern California and the Glenn County area, tick-borne disease is not a theoretical risk; it is a practical one. These infections matter for auto-immune blood disorders because they can directly trigger or mimic immune-mediated destruction of blood cells, sometimes making it impossible to distinguish primary auto-immune disease from infection-triggered disease without comprehensive testing.
Tick-borne diseases that affect blood:
- Lyme disease: can trigger immune reactions affecting blood and joint health
- Rocky Mountain spotted fever: causes serious blood vessel and platelet damage that can look like primary IMT
- Ehrlichia and Anaplasma: both target white blood cells and platelets; ehrlichiosis specifically can be clinically indistinguishable from primary IMTP without a tick panel
- IMHA secondary to Babesia: Babesia parasites invade red blood cells and simultaneously provoke immune-mediated destruction, a classic example of infection-triggered secondary IMHA
This is why tick-borne disease testing is a standard component of our auto-immune blood disease workup at Mid-Valley Veterinary Hospital. Treating what looks like a primary auto-immune condition without screening for an underlying infection can lead to incomplete treatment and relapse.
The Diagnostic Workup: What to Expect
Walking into an evaluation for suspected auto-immune blood disease can feel overwhelming. Here is what the process typically involves:
- History and physical exam: When did symptoms start, how quickly have they progressed, any known tick exposure, recent medications, appetite and water consumption changes. Physical exam focuses on gum color, signs of bruising or petechiae, heart and lung sounds, and overall comfort.
- Complete blood count (CBC) and blood smear: Quantifies red blood cells, white blood cells, and platelets. Microscopic examination of the smear reveals signs of immune-mediated destruction such as agglutination (clumping of red cells) and spherocytes.
- Coombs test: Detects antibodies attached to red blood cell surfaces, directly confirming immune-mediated destruction.
- Reticulocyte count: Measures whether the bone marrow is actively generating new red blood cells in response to the destruction.
- Chemistry panel: Evaluates kidney and liver function to guide medication selection and identify organ involvement.
- Tick-borne disease panel: Tests for Lyme disease, Ehrlichia, Anaplasma, Babesia, and other tick-transmitted infections that may be driving or complicating the disorder.
Our diagnostics include an in-house lab with approximately 20-minute turnaround for most panels, cytology reviewed by board-certified pathologists via AI-assisted microscope, and reference lab coordination for specialized testing. This means we are not waiting days to begin treatment.
Treatment: Stopping the Attack and Supporting the Body
Treatment has two parallel goals: stopping the immune attack and supporting your pet while blood counts recover. Many pets begin treatment in a hospital setting and transition home as they stabilize.
Primary treatment approaches:
- Corticosteroids: The cornerstone of immunosuppressive therapy; slows or stops the immune attack on blood cells
- Additional immunosuppressants: Added when the steroid response is insufficient or side effects limit dosing
- Supportive care: IV fluids, oxygen supplementation if breathing is labored, stomach protectants for steroid-related GI effects
- Anti-clotting medications: For IMHA patients identified as high-risk for thrombosis
- Antimicrobials: Targeted to the specific tick-borne organism when infection is confirmed as a trigger
Blood transfusions are sometimes needed to bridge severely anemic patients while treatment takes effect. Immune-mediated disease treatment is highly individualized, and protocols are adjusted based on how each patient responds.
Recovery typically takes weeks to months, with gradual medication tapering as blood counts stabilize. Relapses can occur, making regular monitoring a long-term commitment for many affected pets.
Tick Prevention as a Frontline Defense
Given the direct link between tick-borne disease and secondary blood disorders, consistent tick prevention is one of the most practical things you can do to protect your pet. In Northern California’s rural areas, tick exposure is a year-round reality, not a seasonal concern.
Tick prevention through veterinarian-recommended prescription products is significantly more reliable than OTC options, particularly in areas with high tick pressure. Year-round prevention eliminates the gaps where tick-triggered blood disorders most commonly develop. Our wellness and preventive care includes tick prevention guidance and annual tick-borne disease screening for at-risk patients.
Warning Signs That Need Same-Day Attention
Auto-immune blood diseases can escalate from subtle to critical in hours. Do not wait for a scheduled appointment if your pet is showing any of these signs:
- Sudden weakness, unsteadiness, stumbling, or collapse
- Pale, white, or yellowish gums
- Unexplained bruising or pinpoint spots on the skin or gums
- Rapid or labored breathing at rest
- Dark, discolored, or blood-tinged urine
- Lethargy so significant your pet will not rise
Call us at (530) 865-5634 during our open hours (Monday through Friday, 8am to 5:30pm) and describe what you are seeing. If your pet is in acute distress outside those hours, seek the nearest emergency facility.
Frequently Asked Questions About Auto-Immune Blood Diseases
What is the difference between anemia and thrombocytopenia?
Anemia is a low red blood cell count that impairs oxygen delivery, causing fatigue, pale gums, and labored breathing. Thrombocytopenia is a low platelet count that impairs clotting, causing bruising, bleeding, and petechiae. Both are serious; both require prompt evaluation. Some pets develop both simultaneously (Evans syndrome).
Can these conditions be cured?
Some pets achieve sustained remission and can eventually be tapered off medication entirely. Others require long-term low-dose maintenance therapy to prevent relapse. Individual response varies significantly, and regular monitoring guides the timeline.
Is my pet contagious if they have IMHA or IMTP?
No. Primary auto-immune blood diseases are not contagious between animals or between animals and people. Tick-borne diseases that trigger secondary forms are transmitted by ticks, not directly between pets.
How quickly do these conditions progress?
Rapidly. IMHA in particular can move from mild to life-threatening within days. Any time you see pale gums, significant lethargy, or labored breathing, same-day evaluation is the right call.
Do dogs or cats that have had IMHA or IMTP need ongoing monitoring?
Yes. Even pets that achieve full remission benefit from periodic blood work to catch any early signs of relapse. We work with each family to build a monitoring schedule appropriate to their pet’s history and response.
Getting to the Right Answer, Quickly
Watching a pet become seriously ill without knowing why is frightening, and the uncertainty is often harder than the diagnosis itself. At Mid-Valley Veterinary Hospital, our diagnostic capabilities are designed to cut through that uncertainty as quickly as possible so that treatment can begin while there is still the most time to work with.
If your pet is showing any warning signs of a blood disorder, contact us right away. For less urgent concerns or to schedule routine screening, you can also reach us at (530) 865-5634. We are here for your family.





Leave A Comment